|
Health
Care – An Imperative
After a year of intense struggle and preparation,
the Vermont Ecumenical Council affirmed this paper on Wednesday,
February 4, 2004. The Trustees thank everyone who contributed to
this effort: the Peace, Justice and Integrity of Creation Committee
(who initiated the concern), the Faith and Order Committee, and
a number of community and health care resource persons.
This paper is offered for study and reflection within
the local church and in ecumenical and community based settings.
Each section of the paper intends to provide basic information or
perspectives, and to open the door for an expanding conversation.
This paper is offered for advocacy and action. The
initial part of the paper seeks to spark an increasing awareness
and knowledge of the roles of faith and communities of faith in
health care. The remaining portion of the paper attempts to lay
out a framework for the long-term engagement demanded by the complex
issues involved in addressing health care. The Touchstones are snapshots,
descriptive pictures, held up before us in the midst of the struggle
to secure a more just system of health care.
This paper is but a beginning for the conversation.
Other resources will be prepared and shared on this topic. The Trustees
invite anyone who reads and is engaged by this paper to join in
the dialogue and action. Responses and questions can be emailed
to the VEC office or call the
office
at 802-434-7307.
This resource (and future pieces) can be found on
the website of the Vermont Ecumenical Council – www.vecbs.org
Introduction
For Christians, the assertion that accessible, affordable
and equitable health care for all is a moral imperative rooted in
Scripture and in our history.
Our member churches have long, distinguished histories
of assisting their member families by sharing in the responsibility
of caring for the sick and those in need. Health care has evolved,
however, from the use of common remedies to a complex and expensive
technology. New medical advances, along with numerous regulations,
bring with them new challenges as to how to deliver health care
for everyone in a fair and all-inclusive way. In the 21st century,
there is no agreement on how to accomplish this goal.
The central dilemma - Whose job is it to provide
health care? Who pays and how? How much responsibility can or should
an individual or family absorb? To what extent is the ‘public’
responsible? To what extent is it acceptable to profit from the
sick? The United States, along with countries all over the world,
are still struggling with these issues.
It is safe to say that the Christian and moral imperatives
are not being met. All persons of compassion are called to join
together in bringing about accessible, affordable and equitable
health care for all.1 One church document states, “Churches
historically have pioneered caring responses of hospitality, health
care and recovery, not just for Christians, but for the whole society.
The church has never sought to take over this responsibility in
society, but rather to encourage the whole society to be responsible
for the health of all.”
The Scriptural Basis
The prophetic witness of the Hebrew Scripture repeatedly
emphasizes that “God.. executes justice for the oppressed;
gives food to the hungry.. lifts up those who are bowed down.. [and]
upholds the orphan and the widow..” (Psalm 146) and asks “what
does the Lord require of you but to do justice, and to love kindness?”
(Micah 6:8)
Jesus continues this witness, challenging a rich
man to put justice and relationship with others first and “sell
all that he owns, and give the money to the poor” (Mark 10:21).
When asked what is the greatest commandment, Jesus includes love
for the neighbor (Mark 12:31). When teaching about the faithful
life which characterizes the renewed, reconciled and transformed
realm of God, Jesus commends those who care for the sick (Matthew
25:31-40). For Christians, providing care of the sick is not optional
– it is an imperative of justice as well as charity.
Christ invites his disciples to follow him in sacrificial
living, opening up a new outlook on illness and health. Matthew’s
citation of Isaiah 53 (the suffering servant), at the end of Jesus’
first day of miracle working, suggests that his own solidarity with
those who are ill is the beginning of their healing, and that the
kenosis (‘emptying’) of his incarnation, leading to
the obedience of his death is what makes him the author of life
for all. Christ invites the Christian to share in his own ministry
of healing and compassion (Mark 6:12-13). Christ promises the power
of healing as a central ingredient of his mission and as a sign
of his identity (Mark 16:17-l8, Luke 10:1-9, Acts 4:12). Healing
is an essential feature of the Jubilee (Luke 4:18-19), the radical
restoration of the world as God intended it to be. And so, Christ
commands us “heal the sick” (Matthew 10:8).
The early church took up the imperative of Christ.
St. James writes that faith without action is dead (James 2:17).
He identifies the destructive effects of wealth and self-indulgence,
and the injustice these cause the innocent. He invites repentance
from the sinner, patience and compassion from the injured, and actions
of reconciling love (James 5:1-11). In this context, St. James instructs
Christians to address their troubles and sicknesses to the elders
of the church, who are to anoint (which was the medical treatment
of the day), pray over and forgive them. By these means, God will
heal (James 5:13-16).
Over the centuries, the churches have taken up these
responsibilities. In various ways, they have practiced liturgical
and sacramental means of forgiveness and healing, including anointing
with oil, prayer and reconciliation. Our churches have also created
and sustained institutions, orders, and schools devoted to hospice,
medical care, hospitality, nursing and related ministries, and sciences.
The History
In the 4th century, St. Basil established health
clinics designed to offer healing to as many persons as possible.
In fact, contemporary scholarship suggests that the early church
employed healing in a radically broad and effective way in the Roman
Empire and beyond. In the centuries that followed, diaconal ministries
within almost every Christian tradition have provided charitable
medical care to the disadvantaged and marginalized.
In 1883, Germany’s Bismark mandated the first
national system of compulsory sickness insurance. Other European
countries began organizing strong incentives for “social insurance
against the chief risks that interrupted continuity of income: industrial
accidents, sickness and disability, old age and unemployment.”
As a decentralized United States shunned national
benefits (except for veterans and seamen), health care remained
private or under the auspices of religious sponsorship. Methodists,
Presbyterians, Episcopalians, Lutherans, Roman Catholics and Jewish
groups and congregations were in the forefront of providing health
care through hospitals, hospices, parish nursing, clinics and a
variety of other programs, including health insurance group programs.
In the 1940s, employers, faced with salary freezes, added health
insurance benefits to employee compensation. Through an economic
expedient, employer-based health insurance became the national standard.
The social justice and civil rights activity of
the 1960’s exposed the plight of significant segments of the
population being denied adequate health care access. Religious leaders
joined others in calling for expansions of public health programs
throughout the country. After failed attempts in the 1930’s
and 1950’s, Congress passed national programs of Medicaid
and Medicare providing the poor as well as the elderly and disabled,
respectively, access to private health care. An additional national
plan failed in the early 1990's, leaving each state to patch together
increasingly expensive care for the uninsured and underinsured.
Today, a significant number of businesses are downsizing and employment-based
benefits are threatened. Our health care system is in an economic
and ethical crisis. The Christian and moral imperatives are still
not being met.
The Context
It is time to examine the conditions compelling
us to act now, and to search for new ways to “work toward
a healthy society of whole persons.”
- Connections -
Millions of people with good health insurance and good connections
to our health care system receive excellent care in the United
States and in Vermont. Millions of others, 15% nationally and
10% of Vermonters2, have no insurance or good connections. Almost
everybody gets some kind of health care someplace, but without
insurance, it will probably be the most expensive and fragmented
kind of care.
- Per Capita Costs - The United States does not provide health care for all of its
citizens, even though it spends twice the average per capita amount
for health care of all other industrialized nations.3 Vermont
health care costs were $2.9 billion in 2003; in a state of roughly
600,000 people, that is nearly $5000 per person. Public funds
currently pay over half of the health care bill.4
- Real Costs -
To contain cost, we must look beyond the price of insurance premiums
to the expenses of care itself. We often think of health care
as a commodity (such as a car). If it isn’t used it won’t
cost us anything.5 Yet, 70% of the health care dollar goes to
the infrastructure providing these services. Vermont infrastructure
includes 14 hospitals, 44 nursing homes, 13 home care agencies,
and over 28,000 health care workers. 80% of these costs are fixed.
Buildings, equipment and salaries must be paid for whether they
are used or not.6 For example, an unoccupied bed costs 80% of
an occupied bed. If the infrastructure is too large, cost continues
for the unused portion; if it’s too small, access is limited,
and waiting lines form.
- Available Services - Individual insurance coverage is usually considered a guarantee
of needed care, but individual coverage does not guarantee that
health care infrastructure services will be available or adequate
when needed. When fixed costs are not met, there are four courses
of action to take: cut services (which will limit access and create
waiting lines); cut staff (which will lower quality of care);
cut administrative costs (which will take legislation to simplify
the system); or shift the cost to other payers (which is our current
policy). We need a system that sustains our services.
- Administrative Costs -
These consume up to 31% of each dollar. The number of administrators
grew 2000% in past thirty years to manage the complex insurance
system. In the same period, the number of nurses grew 159% and
the demand for nursing care is not being met.7
- Drug Costs - There has been no control over yet another of the fastest growing
costs – pharmaceutical drugs. The recent federal Medicare
Prescription Act fails to contain prescription costs.8 While many
believe that the pharmaceutical industry carries the burden of
investing in research for life-saving drugs, the companies: a)
spend more on marketing than research; b) spend no more than the
European countries to put out the same number of new drugs a year;
and c) have more profits than all other Fortune 500 companies.9
For-profit health care and insurance corporations have not produced
affordable care while maintaining profits from the sick. The price
of health insurance covers more than health care when up to 35%
goes for overhead and profits.10
- Health Outcomes - Spending the most money in the world has not brought the United
States the best results in health care outcomes such as length
of life. American women are 20th out of 29 which is particularly
disappointing since we were first in 1945, just as other nations
began to make great strides in providing universal health care.
Having the world’s leading technological advances and performing
the second largest number of procedures (Japan is first) has not
produced the best outcomes in the world.11
- Wellness - Although insurance is described as covering health care, benefits
are often limited to sick care without support for prevention
and wellness measures.
- Equity - There are growing gaps in health care equity. In the United
States, working Americans 18 to 64 years old were more likely
to have health insurance (82%) than non-workers (74.3%).12 There
is a growing gap between market expectations for delaying aging
and enhancing healthy natural aging. There is a growing gap between
national priorities for spending and citizen priorities, as 72%
of Americans agree that the government should provide universal
health care, even if it means repealing most tax cuts passed since
2000.13
- Employer-based insurance - This benefit is threatened as employers face both rising costs
and contentious employee benefit negotiations. Many employers
offer part-time jobs to avoid paying for benefits. Employees are
trapped in jobs to keep their benefits without guarantees that
the jobs will last. Businesses are questioning the value of employer-based
health care and feel a progressive payroll tax along with individual
income taxes would provide more stable funding.14
- State health insurance - Vermont has patched together one of the best state health insurance
programs for the uninsured and underinsured in the nation but
the patches are being stretched by rising costs and falling tax
revenues. Further, accessing the patches often involves confusing,
complicated negotiations for both the consumers and the providers.
- Unaware - Many people have not experienced the current conditions in health
care and do not realize at this point that coverage is not always
affordable, accessible and equitable.
The Conversation
While this paper is a call to action, it is also
a call for reflection and dialogue on authentic moral boundaries
and the inner moral principles of health care acts. This is necessary
for the household of faith to understand its foundations for approaching
health care issues and, together with other communities and agents
of community in our world, to identify an ethical/moral framework
that can guide public policy and individual initiatives.
A first step is to speak together about the meaning
of “health”. It is not enough to equate “health”
with “human happiness” (“if you have your health,
you have everything”). At the same time, “health”
can not be the broad label for every human flourishing. We must
not “medicalize” the whole of human experience. The
World Health Organization (WHO) defined health “as a state
of complete physical, mental, and social well-being, and not merely
the absence of disease or infirmity.”
A second step can be to acknowledge that “health
care” itself can be ambiguous in meaning. Do all the actions
taken in the name of “health care” serve the restoration
of health and the alleviation of symptoms? Nor can we lose sight
of the impact of personal activities such as eating as we should
and exercise. Add issues of the quality of housing, water, sewage
and the environment, and it becomes clear that “health care”
is a complex interrelationship between health and other aspects
of human well-being.
A third step is to understand and agree that health
care in all its dimensions cannot be separated from an ethical and
religious context. A health care paradigm that would implicitly
or explicitly close itself off from the Transcendent and which would
accept principles based only on social and political consensus would
be irresponsible and unacceptable. Health care ethics like bio-ethics
must be grounded on objective truth, not ideologies or subjective
opinions.
Within such an ethical framework some things proposed
as integral to health care – objectives or procedures –
must be questioned and even excluded. This even if they pass the
test of public opinion or a calculus of good over bad consequences.
Not everything we might desire that appears good is morally good.
Furthermore, the so-called “technological imperative”
has its moral limits.
This conversation needs to include careful distinctions
between health care “resources” and health care “systems”.
A health care system may be a mixture or combination of public and
free as well as public but for charge. It may be joint public and
private, private but regulated, and private and unregulated. It
is in fact the whole complex of resources, institutions, policies,
practices, persons and actions that provide health care in a particular
community.
Critical to this conversation is the issue of allocation.
This includes the notion of “rationing” and “prioritization”.
There needs to be an awareness of implicit and explicit decision
making, and a straight forward look at what have become the three
standard responses to availability of resources: “spend more”,
“be more efficient” and “distribute better”.
The meaning of justice is a central issue. There
are many theories of morality and of justice. What is involved in
reaching accepted choices on issues of justice? As Christians we
should strive for the widest meaning of justice (what is “due”
to the other) and reject attempts to separate justice from love
and mercy. We find in the “Good Samaritan” (Luke 10:25-37)
a model for allocation - one of “rescue” and “inclusiveness”.
Any health care system that stems from or deepens social, financial
or ethnic divisions is to be regarded as not in the spirit of Jesus.
Attention needs to be given to the example of the “Wise Steward”
(Mt. 24:45; Mt. 10:16; 25:1-13; 25:14-30). We should also include
in our model “an option for the poor” as a special instance,
not necessarily covered by justice and equality. Any health care
system that rests upon profit of the few from the suffering of the
many is not in the spirit of Jesus. All this needs to be part of
the ongoing discussion related to the identification of needs.
The Touchstones
A touchstone, in an earlier mining era, was a hard
black stone used as a standard for assessing the quality of gold
or silver in other stones. Here we hold up three qualities as touchstones
for testing the pursuit of a health care system to serve all Vermonters.
Affordable
There should be no financial barriers to individual
health care. An affordable health care system assures fair financing
with cost controls that establish reasonable, uniform rates for
sustaining services and obtaining supplies without exceeding the
level of inflation.
Recognizing that financial resources are finite,
an affordable health care system requires the authority to solve
problems while being accountable to all Vermonters. Controlling
cost demands good business practices: monitoring care expenses and
instituting efficiencies (such as simplifying administrative costs);
planning an infrastructure and services that match Vermonters’
health care needs; setting a budget with fair reimbursement that
adequately meets fixed expenses; negotiating uniform fees and prices
with providers and pharmaceutical suppliers; and guaranteeing an
end to cost-shifting because every Vermonter is a paying patient.15
Accessible
An accessible Vermont health care system establishes
life-long benefits without discrimination because of age, income,
employment or prior medical conditions.16 The benefit plan pays
for as many medically necessary services of proven value in promoting
health and relieving suffering as Vermont can afford. It allows
for free choice of a qualified health care provider and facility.
It plans for sustainable infrastructure services to meet Vermonters’
needs. In a just society, the health of individuals depends upon
the health of the society and community. The community has access
to an accounting of the health care system’s resources, financing
and quality of care.
Equitable
Health care is a shared service, a public good.
Like fire and police protection, roads and defense, it is something
we all need, but cannot provide by ourselves.
An equitable health care system recognizes that
health care services and infrastructure are shared: when one person
isn’t using them, someone else is. We know that 10% of Americans
(in fact, most populations) use 73% of the health care dollar at
one time while 80% of Americans use only 15% over a lifetime.17
Assuming personal responsibility for achieving good health, prevention
and early detection delays entry into the 10% group but nearly everyone
will be there at some point during their lifetime.18 Providing high
quality chronic disease care, hospice and home care helps to control
the 10% group costs.19
An equitable health care system acknowledges that
the primary function of health care payments is to maintain quality
infrastructure and services as well as care of an individual. It
reimburses providers (nurses, housekeeping staff, hospitals, as
well as doctors) because they deserve to be paid fairly for their
knowledge, work and time. When everyone pays, cost-shifting is eliminated
and payment sustains the service.
Believing that health comes from spiritual
as well as clinical healing, the Vermont Ecumenical Council calls
upon its clergy and congregations to become knowledgeable regarding
these issues, take responsibility for personal and family well-being,
and encourage their communities to continue their tradition of justice.
Vermont has a tradition of bold initiatives. It was the first state
to ban slavery,20 and to promote public education.21 Vermont could
again be a leader in the nation by guaranteeing health care for
every citizen.
1 Vermont Health Care for All, Inc. Although
universal health care systems vary throughout the world, they have
these features in common.
2 Vermont data 2002
Insurance status || total population || %
of population
Fully Insured || 209,433 || 34.0%
Self-Insured || 151,594 || 24.6%
PRIVATE TOTAL || 361,027 || 58.6%
Medicaid || 102,736 || 16.7%
Medicare || 91,170 ||14.8%
Uninsured || 61,659 ||10.0%
POPULATION || 616,592 || 100.0%
Vermont Annual Statement Supplement Report, BISHCA
3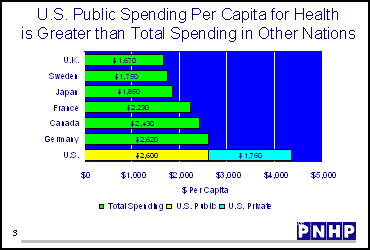
4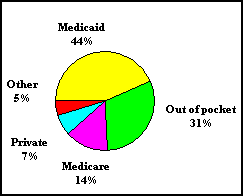 A
good example of this is a view of who pays for care in Vermont’s
nursing homes. A
good example of this is a view of who pays for care in Vermont’s
nursing homes.
5 Harris Poll, 10.03. 62% of Americans consider health care a public
good; 32% think of it as a private product to purchase. The question
posed was: Should health care be a public good or a private economic
good?
6 Richter, Rothwell and Doran. A New Perspective
on Health Care. Vermont Health Care for All, Inc. (VtHCA)
7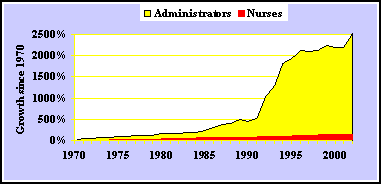
8 Medicare Prescription Drug Benefit Act does
not add prescription benefits to Medicare. It provides a marketing
opportunity for insurance companies to sell a supplemental policy
for prescription drugs, prohibits bulk-buying or negotiating a lower
cost from pharmaceutical corporations, and subsidizes the insurance
and pharmaceutical corporations for some low income seniors.
9 Several sources of pharmaceutical industry
economics are readily available. Two major ones are: “Prescription
Drugs Policy Toolkit,” Center for Policy Alternatives. Marcia
Angell, “The Pharmaceutical Industry – to whom is it
accountable?” New England Journal of Medicine, 2000.
10 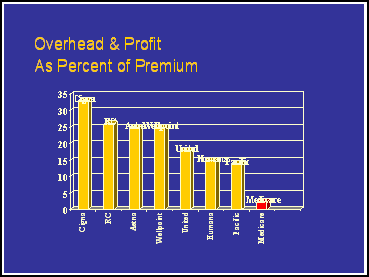
11 There are many examples such as length of
life noted above but this ten year old statistic still stands; patients
in U>S> get more heart procedures than patients in Canada,
but their death rates from heart disease are the same. New England
Journal of Medicine, 1993.
12 U.S. Census Report 2002
13 Pew Research Center 8/03
14 Vermont Businesses for Social Responsibility
Policy Statement on Universal Health Care for Vermont, 2001.
15 Richter, Rothwell and Doran. A New Perspective
on Health Care. Vermont Health Care for All, Inc. (VtHCA).
16 United Methodist Book of Resolutions, p.
274 adds: as to economic status, mental or physical disability,
geographic location, race, color, religion, sex, national origin
or language.
17 Agency for Healthcare Research and Quality.
1999
18 A new way of viewing health care insurance
calls for payments to maintain services and infrastructure instead
of care for an individual. Since the user pays and a non-user may
enter the user category at any time, everyone shares the cost of
maintenance. Richter, Rothwell and Doran. A New Perspective on Health
Care. VtHCA.org website
19 Chronic disease accounts for 78 % of the
state’s health care dollars and 60 % of an individual’s
health care dollars are spent in the last six weeks of life. BISHCA.
20 Toward Racial Equality: Harper’s weekly
reports on black America, slavery timetable.
1777 - Vermont amends its constitution to ban slavery. Over the
next 25 years, other Northern states emancipate their slaves and
ban the institution: Pennsylvania, 1780; Massachusetts and New Hampshire,
1783; Connecticut and Rhode Island, 1784; New York, 1799; and New
Jersey, 1804. Some of the state laws stipulate gradual emancipation.
21 In addition to being the first state
to provide for a state university in its constitution, Vermont built
the first land grant college under a national plan conceived by
Vermonter Justin Morrill. The first agricultural college in the
US (as it is known officially, "The University of Vermont and
State Agricultural College"), the first normal school, the
first private military academy (Norwich University) and the first
school specifically established for the college training of women
were also in Vermont. Virtual Vermont Internet Magazine.
|
